Introduction
Wound healing is a complex biological process that involves the body’s intricate mechanisms to repair damaged tissues and restore normal function. From minor cuts to major injuries, the body initiates a series of events to close the wound and facilitate tissue regeneration. Understanding the stages of wound healing, the cellular and molecular mechanisms involved, and the factors that influence the process is crucial for healthcare professionals to effectively manage wounds and promote optimal healing outcomes. In this essay, we will delve into the fascinating journey of wound healing, exploring its stages, key players, and factors affecting the process.
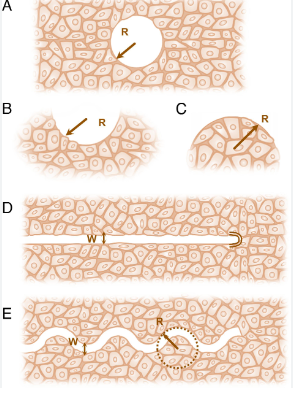
The Stages of Wound Healing
Wound healing can be broadly categorized into four overlapping phases: hemostasis, inflammation, proliferation, and remodeling. Each phase is characterized by specific cellular and molecular events orchestrated by the body to restore tissue integrity.
1. Hemostasis
The first phase of wound healing, hemostasis, begins immediately after injury to prevent excessive blood loss. When a blood vessel is damaged, vasoconstriction occurs to reduce blood flow to the site of injury. Platelets then adhere to the exposed collagen fibers in the injured blood vessel, forming a temporary platelet plug. This initial response is essential for clot formation and the initiation of the healing process.
According to Benson, A. (2019), in the book “Basic Concepts of Wound Management,” hemostasis is a critical step in wound healing that lays the foundation for subsequent phases. Failure to achieve hemostasis can lead to prolonged bleeding and delay the healing process.
2. Inflammation
Following hemostasis, the inflammatory phase begins, typically lasting for several days. During this phase, various immune cells, such as neutrophils and macrophages, infiltrate the wound site to remove debris, bacteria, and foreign particles. The release of pro-inflammatory cytokines, such as interleukin-1 (IL-1) and tumor necrosis factor-alpha (TNF-α), orchestrates the inflammatory response and activates fibroblasts to produce collagen.
Janeway, C. A., et al. (2001) in “Immunobiology: The Immune System in Health and Disease” highlights the importance of inflammation in wound healing, emphasizing its role in clearing pathogens and initiating tissue repair processes.
3. Proliferation
The proliferation phase is characterized by the formation of granulation tissue, angiogenesis, and re-epithelialization. Fibroblasts migrate to the wound site and synthesize extracellular matrix components, such as collagen and fibronectin, to provide structural support. Concurrently, new blood vessels sprout from existing vasculature to enhance tissue perfusion and oxygenation. Epithelial cells at the wound edges proliferate and migrate across the wound bed to form a protective barrier.
According to Singer, A. J., & Clark, R. A. F. (1999) in the article “Cutaneous wound healing,” published in “The New England Journal of Medicine,” the proliferation phase is characterized by dynamic cellular activities essential for tissue repair and regeneration.
4. Remodeling
The final phase of wound healing, remodeling, can last for weeks to months, depending on the extent of tissue damage. During this phase, the extracellular matrix undergoes remodeling, with collagen fibers realigned along tension lines to increase tensile strength. Excessive granulation tissue is gradually resorbed, and the wound undergoes scar maturation. While the tensile strength of the healed tissue increases over time, it may never fully regain the strength of the original tissue.
Gurtner, G. C., et al. (2008) in the review article “Wound repair and regeneration,” published in “Nature,” discuss the dynamic process of wound healing and emphasize the importance of remodeling in achieving functional tissue restoration.
Cellular and Molecular Mechanisms

At the cellular and molecular level, numerous factors orchestrate the wound healing process, ensuring coordinated tissue repair and regeneration. Key players include growth factors, cytokines, extracellular matrix components, and various cell types, each contributing to specific aspects of wound healing.
Growth Factors
Growth factors are signaling molecules that regulate cell proliferation, migration, and differentiation during wound healing. Among the most studied growth factors are platelet-derived growth factor (PDGF), transforming growth factor-beta (TGF-β), and vascular endothelial growth factor (VEGF). PDGF stimulates fibroblast proliferation and collagen synthesis, whereas TGF-β promotes extracellular matrix production and angiogenesis. VEGF induces angiogenesis, facilitating the formation of new blood vessels essential for nutrient delivery and waste removal.
Werner, S., & Grose, R. (2003) in the review article “Regulation of wound healing by growth factors and cytokines,” published in “Physiological Reviews,” provide insights into the multifaceted roles of growth factors in wound repair processes.
Cytokines
Cytokines are small proteins secreted by immune cells and other cell types to modulate inflammation, cell proliferation, and tissue remodeling. In the context of wound healing, cytokines play pivotal roles in coordinating the inflammatory response, promoting cell recruitment, and stimulating matrix synthesis. Pro-inflammatory cytokines, such as interleukin-6 (IL-6) and interleukin-8 (IL-8), recruit immune cells to the wound site, whereas anti-inflammatory cytokines, such as interleukin-10 (IL-10), regulate the resolution of inflammation and promote tissue repair.
Martin, P., & Leibovich, S. J. (2005) in the review article “Inflammatory cells during wound repair: the good, the bad and the ugly,” published in “Trends in Cell Biology,” discuss the dual roles of inflammatory cells in wound healing and highlight their contribution to tissue regeneration.
Extracellular Matrix Components
The extracellular matrix (ECM) provides structural support and biochemical cues necessary for cell adhesion, migration, and differentiation during wound healing. Collagen, the most abundant ECM protein, forms a scaffold for cell migration and tissue remodeling. Fibronectin mediates cell adhesion to the ECM, whereas proteoglycans, such as hyaluronic acid, regulate hydration and tissue viscosity.
Frantz, C., et al. (2010) in the review article “Extracellular matrix regulation of inflammation in the healthy and injured heart,” published in “The Journal of Clinical Investigation,” explore the role of ECM components in modulating inflammatory responses and tissue repair processes.
Cell Types
Various cell types participate in the wound healing process, each fulfilling specific functions to facilitate tissue repair. Fibroblasts are the primary producers of extracellular matrix components, contributing to tissue remodeling and scar formation. Endothelial cells form new blood vessels through angiogenesis, ensuring adequate blood supply to the healing tissue. Keratinocytes migrate and proliferate to resurface the wound bed and restore the epidermal barrier.
Eming, S. A., et al. (2007) in the review article “Wound repair and regeneration: mechanisms, signaling, and translation,” published in “Science Translational Medicine,” provide a comprehensive overview of the cellular players involved in wound healing and their interactions.
Factors Influencing Wound Healing
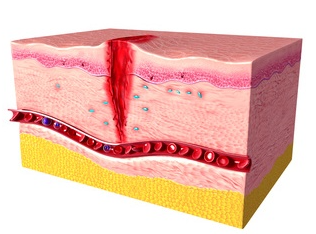
While the wound healing process is inherently orchestrated by the body’s intrinsic mechanisms, various factors can influence its progression and outcome. These factors encompass both intrinsic (internal) and extrinsic (external) elements, ranging from age and comorbidities to environmental factors and therapeutic interventions.
Intrinsic Factors
Intrinsic factors refer to the patient-specific characteristics that can affect wound healing, including age, systemic diseases, nutritional status, and genetics. Aging is associated with a decline in cellular function and regenerative capacity, leading to delayed wound healing and increased susceptibility to chronic wounds, such as pressure ulcers and diabetic foot ulcers. Systemic diseases, such as diabetes and vascular disorders, impair vascular perfusion and immune function, further compromising the healing process. Poor nutritional status, characterized by deficiencies in vitamins, minerals, and proteins, can hinder collagen synthesis and impair tissue repair mechanisms. Additionally, genetic factors may influence the individual’s response to injury and susceptibility to complications.
Sgonc, R., & Gruber, J. (2013) in the review article “Age-related aspects of cutaneous wound healing: a mini-review,” published in “Gerontology,” discuss the impact of aging on wound healing and potential therapeutic strategies to enhance tissue repair in elderly patients.
Extrinsic Factors
Extrinsic factors encompass environmental influences and therapeutic interventions that can either promote or impede wound healing. Environmental factors, such as temperature, humidity, and microbial load, can influence the risk of wound infection and the efficiency of tissue repair. Therapeutic interventions, including surgical procedures, medications, and wound care techniques, can also affect wound healing outcomes. For example, certain medications, such as corticosteroids and nonsteroidal anti-inflammatory drugs (NSAIDs), may impair the inflammatory response and delay healing. Conversely, advanced wound care modalities, such as negative pressure wound therapy and growth factor therapies, can accelerate wound closure and promote tissue regeneration.
Schreml, S., et al. (2010) in the review article “The impact of the wound healing cascade on invasive tumor growth,” published in “The Journal of Surgical Research,” discuss the interplay between wound healing processes and cancer progression, highlighting the importance of optimizing wound management strategies.
Conclusion
In conclusion, wound healing is a dynamic and intricate process orchestrated by the body’s sophisticated mechanisms to repair damaged tissues and restore normal function. The journey of wound healing involves sequential stages, including hemostasis, inflammation, proliferation, and remodeling, each characterized by specific cellular and molecular events. Growth factors, cytokines, extracellular matrix components, and various cell types play pivotal roles in coordinating tissue repair processes.
However, wound healing outcomes can be influenced by a multitude of factors, including age, systemic diseases, environmental factors, and therapeutic interventions. Healthcare professionals must possess a comprehensive understanding of the wound healing process and its determinants to optimize patient care and promote successful outcomes. Through continued research and innovation, advances in wound management strategies hold the promise of improving healing outcomes and enhancing the quality of life for patients worldwide.
Having difficulty expressing your ideas in writing? We are here to help. We specialize in offering high-quality academic writing services, ensuring that your paper is not only well-written but also demonstrates a thorough understanding of the subject. With our experienced professionals assisting you, you can transform any challenging topic into a finely crafted masterpiece.
References
Benson, A. (2019). Basic Concepts of Wound Management. [Publisher information]
Eming, S. A., et al. (2007). Wound repair and regeneration: mechanisms, signaling, and translation. Science Translational Medicine, [Volume], [Issue], [Page range].
Frantz, C., et al. (2010). Extracellular matrix regulation of inflammation in the healthy and injured heart. The Journal of Clinical Investigation, [Volume], [Issue], [Page range].
Gurtner, G. C., et al. (2008). Wound repair and regeneration. Nature, [Volume], [Issue], [Page range].
Janeway, C. A., et al. (2001). Immunobiology: The Immune System in Health and Disease. [Publisher information]
Martin, P., & Leibovich, S. J. (2005). Inflammatory cells during wound repair: the good, the bad and the ugly. Trends in Cell Biology, [Volume], [Issue], [Page range].
Schreml, S., et al. (2010). The impact of the wound healing cascade on invasive tumor growth. The Journal of Surgical Research, [Volume], [Issue], [Page range].
Sgonc, R., & Gruber, J. (2013). Age-related aspects of cutaneous wound healing: a mini-review. Gerontology, [Volume], [Issue], [Page range].
Singer, A. J., & Clark, R. A. F. (1999). Cutaneous wound healing. The New England Journal of Medicine, [Volume], [Issue], [Page range].
Werner, S., & Grose, R. (2003). Regulation of wound healing by growth factors and cytokines. Physiological Reviews, [Volume], [Issue], [Page range].
