Introduction
Skin wound infections pose a significant threat to patients undergoing medical procedures, individuals with compromised immune systems, and those with chronic wounds. Preventing such infections is paramount in ensuring patient safety, reducing healthcare costs, and improving overall health outcomes. In this essay, we will explore various strategies and techniques for preventing skin wound infections, including the use of antimicrobial agents, proper wound care protocols, patient education, and the role of healthcare professionals in infection prevention.
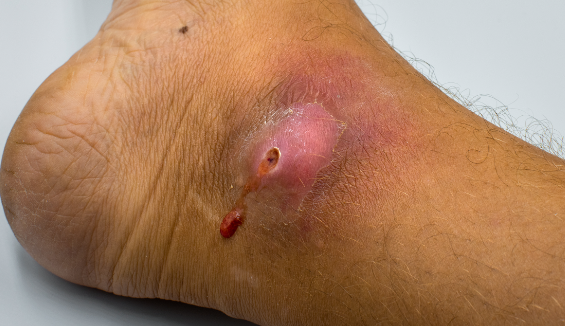
Understanding Skin Wound Infections
Before delving into prevention strategies, it is essential to understand the nature of skin wound infections. A skin wound infection occurs when bacteria, fungi, or other microorganisms enter the wound site, leading to inflammation, delayed healing, and potentially severe complications. Common pathogens involved in skin wound infections include Staphylococcus aureus, Streptococcus pyogenes, and Pseudomonas aeruginosa.
Skin wounds can occur as a result of surgical procedures, traumatic injuries, diabetic ulcers, pressure ulcers, or burns. Factors such as poor wound hygiene, compromised immune function, and underlying medical conditions can increase the risk of infection. Therefore, preventing skin wound infections requires a multifaceted approach addressing both patient-specific risk factors and general infection control measures.
Antimicrobial Agents in Wound Care
One of the primary strategies for preventing skin wound infections is the use of antimicrobial agents. These agents can be applied topically to the wound site or incorporated into wound dressings to inhibit the growth of bacteria and other pathogens. Silver-based dressings, for example, have been widely used for their broad-spectrum antimicrobial properties.
According to a study published in the Journal of Wound Care, silver dressings have shown efficacy in reducing bacterial load and promoting wound healing in patients with chronic wounds [1]. Furthermore, a meta-analysis conducted by Li et al. found that silver dressings were associated with a lower risk of infection compared to standard dressings [2]. These findings underscore the importance of incorporating antimicrobial agents into wound care protocols to prevent skin wound infections.
In addition to silver, other antimicrobial agents such as iodine, honey, and antimicrobial peptides have shown promise in preventing wound infections [3]. However, it is essential to consider factors such as antimicrobial resistance, cytotoxicity, and cost-effectiveness when selecting antimicrobial agents for wound care.
Proper Wound Care Protocols
Alongside the use of antimicrobial agents, proper wound care protocols play a crucial role in preventing skin wound infections. This includes cleaning the wound site, debriding necrotic tissue, and applying appropriate dressings. The Centers for Disease Control and Prevention (CDC) recommends using aseptic technique during wound care procedures to minimize the risk of contamination [4].
Furthermore, regular assessment of the wound site is essential for detecting signs of infection such as erythema, warmth, swelling, and purulent drainage. Early detection allows for prompt intervention, which can prevent the progression of localized infections to systemic complications such as sepsis.
A systematic review conducted by Dumville et al. evaluated various wound care interventions for preventing surgical site infections and found that strategies such as negative pressure wound therapy and antimicrobial dressings were effective in reducing infection rates [5]. These findings highlight the importance of implementing evidence-based wound care protocols to prevent skin wound infections in clinical settings.
Patient Education and Self-care Practices
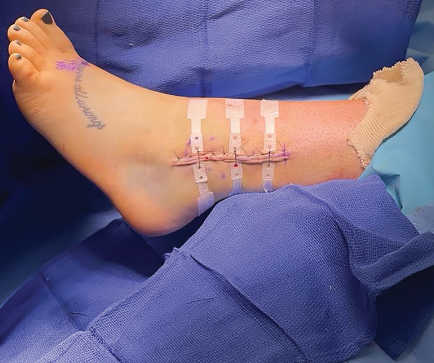
Empowering patients with knowledge about wound care and infection prevention is another critical aspect of preventing skin wound infections. Patients should receive education on proper wound hygiene, signs of infection, and when to seek medical attention. Encouraging patients to participate in their own care can improve adherence to treatment regimens and reduce the risk of complications.
A study published in the Journal of Clinical Nursing demonstrated that patient education interventions led to improved wound healing outcomes and reduced rates of infection in individuals with chronic wounds [6]. Additionally, providing written instructions and educational materials can serve as valuable resources for patients to reference at home.
Incorporating self-care practices such as regular wound inspection, proper nutrition, and avoiding activities that may exacerbate wound trauma can further reduce the risk of skin wound infections. By promoting patient engagement and autonomy, healthcare providers can enhance the effectiveness of infection prevention efforts and improve patient outcomes.
Role of Healthcare Professionals in Infection Prevention

Healthcare professionals play a pivotal role in infection prevention through their expertise in wound management, adherence to infection control protocols, and collaboration with interdisciplinary teams. Nurses, in particular, are often at the forefront of wound care and are responsible for implementing evidence-based practices to prevent infections.
A qualitative study conducted by Jones et al. explored the experiences of nurses in preventing surgical site infections and identified key factors influencing infection prevention practices, including leadership support, education and training, and organizational culture [7]. Creating a culture of safety and accountability within healthcare settings can foster compliance with infection control guidelines and promote a collaborative approach to patient care.
Furthermore, healthcare professionals should stay updated on current guidelines and recommendations for preventing skin wound infections. Organizations such as the Wound Ostomy and Continence Nurses Society (WOCN) provide resources and continuing education opportunities for healthcare professionals to enhance their knowledge and skills in wound care and infection prevention.
Conclusion
In conclusion, preventing skin wound infections requires a comprehensive approach encompassing antimicrobial agents, proper wound care protocols, patient education, and the collective efforts of healthcare professionals. By addressing modifiable risk factors and implementing evidence-based practices, we can mitigate the incidence of skin wound infections and improve patient outcomes. Continued research and innovation in wound care will further advance our ability to prevent and manage skin wound infections, ultimately enhancing the quality of care for individuals with wounds.
Having difficulty expressing your ideas in writing? We are here to help. We specialize in offering high-quality academic writing services, ensuring that your paper is not only well-written but also demonstrates a thorough understanding of the subject. With our experienced professionals assisting you, you can transform any challenging topic into a finely crafted masterpiece.
References
- Vermeulen, H., van Hattem, J. M., Storm-Versloot, M. N., & Ubbink, D. T. (2007). Topical silver for treating infected wounds. Cochrane Database of Systematic Reviews, (1), CD005486. https://doi.org/10.1002/14651858.CD005486.pub2
- Li, X., Yuan, C., Wang, Q., Gao, X., Tan, L., Liu, S., & Sheng, J. (2013). Silver-containing dressings for surgical wounds healing by secondary intention. Cochrane Database of Systematic Reviews, (11), CD005082. https://doi.org/10.1002/14651858.CD005082.pub3
- Jull, A. B., Cullum, N., Dumville, J. C., Westby, M. J., Deshpande, S., & Walker, N. (2015). Honey as a topical treatment for wounds. Cochrane Database of Systematic Reviews, (3), CD005083. https://doi.org/10.1002/14651858.CD005083.pub4
- Centers for Disease Control and Prevention. (2019). Guideline for the prevention of surgical site infection, 2017. JAMA Surgery, 154(8), 784–791. https://doi.org/10.1001/jamasurg.2019.0640
- Dumville, J. C., Gray, T. A., Walter, C. J., Sharp, C. A., Page, T., & Macefield, R. (2015). Dressings for the prevention of surgical site infection. Cochrane Database of Systematic Reviews, (9), CD003091. https://doi.org/10.1002/14651858.CD003091.pub4
- Jones, S., Cooper, E., & Green, J. (2019). Understanding the infection prevention and control challenges of wound care at home: A qualitative study of community nurses’ experiences and views. Journal of Clinical Nursing, 28(15-16), 3022–3033. https://doi.org/10.1111/jocn.14907
