Introduction
In modern healthcare settings, the utilization of Electronic Health Records (EHRs) has become increasingly prevalent, revolutionizing the way patient information is stored, accessed, and utilized. EHRs serve as comprehensive digital repositories that contain patient demographics, medical history, diagnoses, medications, treatment plans, laboratory results, and other relevant clinical data. The integration of EHRs into clinical workflows has the potential to significantly enhance clinical decision-making processes, leading to improved patient outcomes, increased efficiency, and enhanced care coordination. This paper will explore the ways in which EHRs enhance clinical decision-making, the challenges associated with their implementation, and the implications for healthcare professionals and patients.
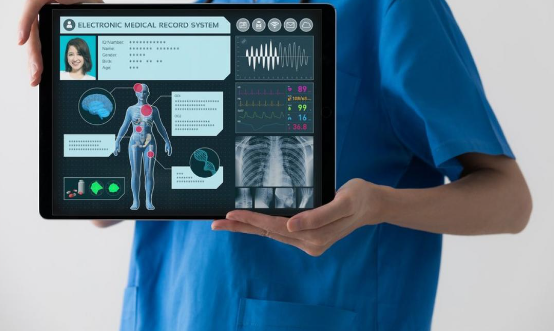
What is An Electronic Health Record (EHR)
An Electronic Health Record (EHR) is more than just a digital version of a patient’s paper chart. Let’s explore its significance:
- Definition: An EHR is a real-time, patient-centered record that contains a patient’s medical and treatment histories, diagnoses, medications, immunization dates, allergies, radiology images, and laboratory results. Unlike traditional paper charts, EHRs go beyond standard clinical data collected in a provider’s office. They provide a broader view of a patient’s care.
- Key Features:
- Real-Time Access: EHRs make information instantly available and secure to authorized users.
- Comprehensive Data: They contain a patient’s complete medical history.
- Decision Support: EHRs offer evidence-based tools for providers to make informed decisions.
- Workflow Automation: They streamline provider workflows.
- Interoperability: EHRs can be shared with other health care providers and organizations, ensuring information continuity across different settings.
- Sharing Across Organizations: EHRs facilitate collaboration among laboratories, specialists, imaging facilities, pharmacies, emergency centers, and workplace clinics. They consolidate information from all clinicians involved in a patient’s care.
- Health IT Advancement: EHRs contribute to building a healthier future by enhancing care coordination and promoting equitable access to health services.
EHRs are essential tools that transcend paper-based records, enabling efficient, informed, and interconnected health care delivery12
Benefits of Electronic Health Records
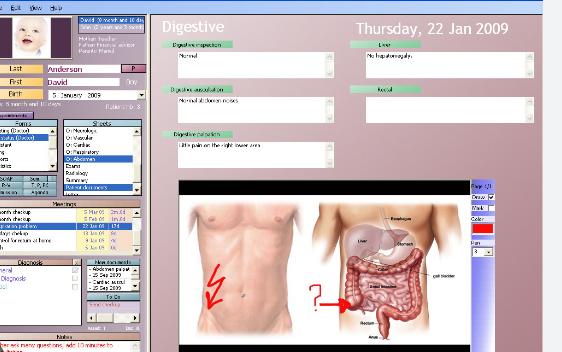
1. Improving Data Accessibility and Availability
One of the primary benefits of EHRs is their ability to centralize patient information, making it easily accessible to healthcare providers across different care settings. Traditionally, paper-based medical records were fragmented and often stored in multiple locations, making it challenging for clinicians to access relevant patient data in a timely manner. With EHRs, healthcare professionals can retrieve comprehensive patient information instantaneously, allowing for more informed clinical decision-making at the point of care.
According to a study by Adler-Milstein et al. (2017), healthcare providers reported significant improvements in their ability to access patient information quickly and efficiently after implementing EHR systems. This increased accessibility of patient data enables clinicians to make more informed decisions regarding diagnosis, treatment options, medication management, and care planning, ultimately leading to improved patient outcomes.
2. Facilitating Information Exchange and Interoperability
In addition to improving data accessibility within individual healthcare organizations, EHRs also facilitate seamless information exchange and interoperability across different care settings. Interoperable EHR systems allow healthcare providers to securely share patient data, clinical notes, and treatment plans with other members of the care team, including primary care physicians, specialists, nurses, and allied health professionals.
A study by Vest et al. (2014) found that interoperable EHR systems were associated with improved care coordination and communication among healthcare providers. By enabling real-time access to patient information across care settings, interoperable EHRs help ensure continuity of care, reduce duplication of services, prevent medical errors, and enhance the overall patient experience.
3. Supporting Evidence-Based Practice
EHRs play a crucial role in supporting evidence-based practice by integrating clinical decision support tools directly into the clinical workflow. These tools provide healthcare providers with real-time alerts, reminders, and recommendations based on clinical guidelines, best practices, and patient-specific data. Clinical decision support alerts may include reminders for preventive screenings, drug-drug interactions, allergy warnings, and evidence-based treatment protocols.
A study by Bright et al. (2012) demonstrated that the use of clinical decision support within EHR systems led to improvements in adherence to clinical guidelines and evidence-based practices. By providing clinicians with timely and relevant information at the point of care, clinical decision support tools help standardize care delivery, reduce variation in practice, and improve the quality and safety of patient care.
4. Enhancing Care Coordination and Continuity
Effective care coordination is essential for optimizing patient outcomes, particularly for individuals with complex medical needs or chronic conditions. EHRs support care coordination efforts by providing a centralized platform for healthcare providers to communicate, collaborate, and share information about patient care plans, transitions of care, and follow-up appointments.
A study by Adler-Milstein et al. (2014) found that healthcare organizations with advanced EHR capabilities, including electronic exchange of patient summaries and care plans, reported improvements in care coordination and patient transitions between care settings. By facilitating communication and information sharing among members of the care team, EHRs help ensure that patients receive timely and appropriate care across the care continuum, leading to better health outcomes and reduced healthcare costs.
5. Challenges and Considerations
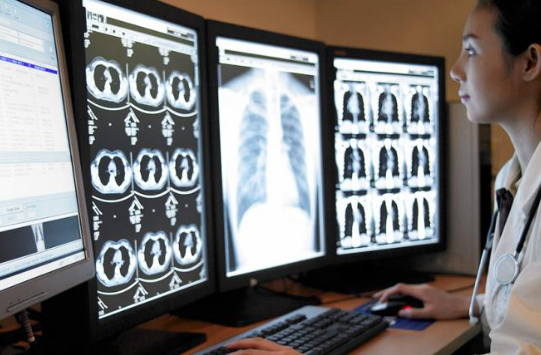
While EHRs offer numerous benefits for enhancing clinical decision-making, their implementation and utilization are not without challenges. One of the primary challenges is the usability of EHR systems, which can vary widely depending on factors such as system design, user interface, and customization options. Poorly designed EHR interfaces can lead to frustration, inefficiency, and clinician burnout, ultimately undermining the potential benefits of EHRs for clinical decision-making.
Furthermore, concerns about data privacy, security, and confidentiality pose significant challenges for EHR implementation. Healthcare organizations must ensure that EHR systems comply with relevant privacy and security regulations, such as the Health Insurance Portability and Accountability Act (HIPAA), to protect patient information from unauthorized access, breaches, and cyber threats.
Additionally, interoperability issues remain a barrier to seamless information exchange and care coordination across different EHR systems and healthcare organizations. Achieving interoperability requires standardized data formats, terminology, and protocols to facilitate the exchange of patient information between disparate systems. Healthcare stakeholders must collaborate to address interoperability challenges and promote the development and adoption of interoperable EHR solutions.
Conclusion
Electronic Health Records have the potential to significantly enhance clinical decision-making processes by improving data accessibility, facilitating information exchange, supporting evidence-based practice, and enhancing care coordination and continuity. By leveraging the capabilities of EHRs, healthcare providers can make more informed and timely decisions, leading to improved patient outcomes, increased efficiency, and enhanced quality of care. However, the successful implementation and utilization of EHRs require careful consideration of usability, privacy and security, interoperability, and other challenges to ensure that EHR systems effectively support clinical decision-making and ultimately improve patient care.
Having difficulty expressing your ideas in writing? We are here to help. We specialize in offering high-quality academic writing services, ensuring that your paper is not only well-written but also demonstrates a thorough understanding of the subject. With our experienced professionals assisting you, you can transform any challenging topic into a finely crafted masterpiece.
