In nursing, pharmacology calculations are the essential skills used to determine the correct dosage and administration method of medications for patients.
Why are they important?
- Patient safety: Accurate calculations are crucial to ensure patients receive the right amount of medication, preventing underdoses, overdoses, and potential harm.
- Effectiveness: Correct dosages maximize the therapeutic benefits of medications and minimize side effects.
- Clinical competence: Calculating medication dosages is a core skill for nurses, demonstrating competence and contributing to safe patient care.
What’s involved?
- Medication orders: Interpreting doctor’s orders and understanding information like prescribed medication, dose, frequency, and route of administration.
- Unit conversions: Converting between different units of measurement (e.g., milligrams to micrograms, milliliters to liters) based on medication concentration and patient weight.
- Dilution calculations: Determining how much medication to add to a diluent (e.g., saline solution) to achieve the desired concentration for administration.
- Infusion rate calculations: Calculating the flow rate for intravenous medications delivered over time.
- Body weight calculations: Using patient weight to adjust medication dosages for personalized needs.
What is the formula for drug calculations for nurses?
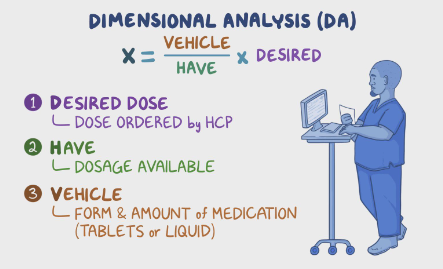
There are various formulas applied depending on the specific scenario and calculation you need to perform. This variability underscores the importance of using reliable resources and double-checking your work to ensure patient safety.
Dose calculation:
- D = (DxV)/H: This formula calculates the dose to be administered, where:
- D = desired dose
- V = volume of available medication
- H = concentration of medication
2. Concentration calculation:
- C = D/V: This formula calculates the concentration of a medication, where:
- C = concentration
- D = desired dose
- V = volume to be administered
3. Infusion rate calculation:
- R = T/V: This formula calculates the infusion rate (flow rate) for medications given over time, where:
- R = rate (e.g., ml/hour)
- T = total volume to be infused
- V = time for infusion
4. Body weight adjustment:
- New dose = (Old dose x New weight) / Old weight: This formula adjusts the dose based on patient weight, where:
- New dose = adjusted dose
- Old dose = prescribed dose
- New weight = patient’s weight
- Old weight = reference weight used for prescribing
What is the 3 step process in calculating dosages?
The three-step process for calculating dosages in nursing can vary depending on the specific scenario and formula used. However, a general guideline for many medication calculations follows these steps:
1. Gather information:
- Medication order: Read the doctor’s orders carefully, noting the prescribed medication, dosage, frequency, and route of administration.
- Medication information: Refer to a reliable medication reference or database to obtain information about the medication’s available strengths, concentrations, and administration considerations.
- Patient information: Consider the patient’s weight, allergies, and any relevant medical conditions that might affect medication dosage.
2. Choose the appropriate formula:
- Based on the information gathered, determine the specific formula needed for your calculation. Common formulas include:
- Dose calculation: D = (DxV)/H
- Concentration calculation: C = D/V
- Infusion rate calculation: R = T/V
- Body weight adjustment: New dose = (Old dose x New weight) / Old weight
- Ensure you understand the variables in the formula and their corresponding units.
3. Perform the calculation and confirm:
- Substitute the gathered information into the chosen formula and solve for the unknown variable.
- Double-check your calculations meticulously, using a calculator or another method for verification.
- If applicable, consider rounding the result according to recommended practices for the specific medication and route of administration.
- Never administer medication based on a single calculation.
- Always have another qualified healthcare professional confirm your final dosage before administration.
What is the formula for IV calculation?
The formula for IV calculations for nurses depends on what you’re trying to calculate. Here are two common scenarios:
1. Calculating the infusion rate:
This determines how quickly a medication is delivered intravenously over a specific time period. The formula is:
R = T / V
Where:
- R is the infusion rate (milliliters per hour, mL/h)
- T is the total volume of fluid to be infused (milliliters, mL)
- V is the time for infusion (hours)
2. Calculating the concentration of a medication for infusion:
This determines how much medication to add to a diluent (carrier fluid) to achieve the desired concentration for administration. The formula is:
C = D / V
Where:
- C is the concentration (milligrams per milliliter, mg/mL)
- D is the desired dose of the medication (milligrams, mg)
- V is the final volume of the infused solution (milliliters, mL)
How do you calculate mg per kg of a drug?
Calculating the mg per kg dose of a drug involves a simple two-step process:
Step 1: Determine the desired total dose in milligrams (mg).
This information should be readily available in the medication order or prescribing guidelines. Make sure you have the correct dose in milligrams (mg), not micrograms (mcg).
Step 2: Divide the total dose (mg) by the patient’s weight in kilograms (kg).
Use the following formula:
mg/kg = Total dose (mg) / Patient weight (kg)
Example:
A doctor prescribes 100mg of medication for a patient who weighs 50kg. What is the mg/kg dose?
Solution:
mg/kg = 100mg / 50kg = 2mg/kg
Therefore, the patient should receive 2mg of the medication for every kilogram of their body weight.
Important notes:
- Always double-check your calculations. Even a small mistake can have serious consequences.
- Use reliable resources for medication information and dosing guidelines, such as drug monographs or clinical practice guidelines.
- Never rely solely on online resources for critical calculations.
- Consider other factors such as the patient’s age, renal function, and other medications they are taking before administering any medication.
- Always consult with a qualified healthcare professional if you are unsure about the correct dosage or have any questions about medication administration.
Resources for Pharmacology Calculations for Nurses:
Drug Information Databases:
- Lexicomp: https://www.uptodate.com/contents/table-of-contents/drug-information
- Micromedex: https://www.micromedexsolutions.com/home/dispatch/
- MedlinePlus Drugs and Medications: https://reference.medscape.com/
Nursing Pharmacology Textbooks:
- Pharmacology and Pharmacotherapeutics for Nursing by Lippincott Williams & Wilkins: https://shop.lww.com/Lippincott-Illustrated-Reviews–Pharmacology/p/9781975170554
- Nursing Pharmacology and Therapeutics by Mosby: https://evolve.elsevier.com/cs/product/9780323092449?role=student
Professional Organizations:
- American Nurses Association (ANA) Center for Medication Safety: https://www.nursingworld.org/~498e32/contentassets/a2ff1bd2d5ca467699c3bc764f7d9198/issue-brief-medication-aides-4-2021.docx
- International Council of Nurses (ICN) Medication Management Resource Centre: https://www.icn.ch/
Calculators and Tools:
- MedMath: https://www.medscape.com/public/medscapeapp
- Nurse Dosage Calculator: https://www.manuelsweb.com/nrs_calculators.htm
- Medscape Drug Interaction Checker: https://reference.medscape.com/drug-interactionchecker
Additional Resources:
- National Council of State Boards of Nursing (NCSBN): https://www.ncsbn.org/
- American Society for Health-System Pharmacy (ASHP): https://www.ashp.org/
- Institute for Safe Medication Practices (ISMP): https://www.ismp.org/
